COVID-19 tests
Executive summary
* The key message from the World Health Organization about COVID-19 has been “test, test, test.”
* While much is being said about testing, less is being said about test reliability.
* There are two key attributes of a medical test – test sensitivity and test specificity. Test sensitivity is the ability of a test to correctly identify those with the disease. Test specificity is the ability of a test to correctly identify those without the disease.
* There are two tests related to COVID-19 that would be extremely useful right now: Test A) Knowing who has the disease (present). Test B) Knowing who has had the disease (past).
* Test A needs to be prepared to diagnose some people with COVID-19 who don’t have it – false positives – to err on the side of caution. Test B needs to be prepared to miss some people who have had COVID-19 – false negatives – to err on the side of caution.
* There is very little evidence on the reliability of Test A. No government in the world has yet rolled out a full programme for Test B.
* “Test, test, test” is the right strategy in principle, but, in practice, test limitations need to be accounted for and other options need to be explored.
Brief update on previous note
Things have moved at quite a pace on masks since my last note. On March 31st, the World Health Organization (WHO) stood by its recommendations that members of the public should not be wearing masks (Ref 1). On April 2nd, news stations around the world reported that the WHO was reviewing the evidence (Ref 2). In the early hours of April 4th, the South China Morning Post reported that the WHO had changed course and now recommended wearing masks in public (Ref 3).
The US Centers for Disease Control and Prevention (CDC) has just issued new advice to wear cloth masks (Ref 4). At the time of writing this, the Deputy Chief Medical Officer for England said that the advice (to not wear a mask) had not changed (Ref 5).
Introduction to this week’s note
Testing is the other hot topic in COVID-19 news. The key message from the WHO conference on March 16th, 2020 was “test, test, test” (Ref 6). This makes sense. We are making huge decisions at the moment with little information and the more information we can gather, the better. However, all medical tests have limitations and we need to be aware of these limitations in the context of COVID-19. This note, therefore, is about the limitations of medical tests generally, what we would like to know about COVID-19 tests and what we may not be able to know for sure.
Test sensitivity and specificity
There are two key attributes of a medical test – test sensitivity and test specificity. They apply to any medical test that aims to diagnose if a person has a condition or not (e.g. cancer screening).
1) Test sensitivity is the ability of a test to correctly identify those with the disease. (The true positive).
2) Test specificity is the ability of a test to correctly identify those without the disease. (The true negative).
The perfect test would be positive in everyone with the disease and negative in everyone without the disease. I’m not aware of any perfect medical test. This is where the terms “false positive” and “false negative” come in. False positive means that someone tests positive who doesn’t have the disease. False negative means that someone tests negative who does have the disease.
I love a good ‘2 by 2’ table and the following one is a useful summary of the four options that can arise from a medical test. The table below has been simplified from an excellent and much cited paper on test sensitivity and test specificity in ophthalmology (Ref 7).
|
Person has the disease |
Person doesn’t have the disease |
|
| Person tests positive |
a) True positive |
b) False positive |
| Person tests negative |
c) False negative |
d) True negative |
The test sensitivity (the ability to identify those with the disease) is a/(a+c) i.e. if C is zero, then a is 100%.
The test specificity (the ability to identify those without the disease) is d/(b+d) i.e. if b is zero, then d is 100%.
Test sensitivity and test specificity are inversely related, meaning that as the sensitivity increases, the specificity decreases and vice versa. To correctly identify as many people as possible who have the disease, it is necessary to accept that there will be false positives and thus to accept a lower test specificity.
Covid-19 tests
There are two tests related to COVID-19 that would be extremely useful right now:
A) Knowing who has the disease (present).
B) Knowing who has had the disease (past).
There are two types of test to assess A and B (Ref 8):
A) Antigen (nucleic acid test).
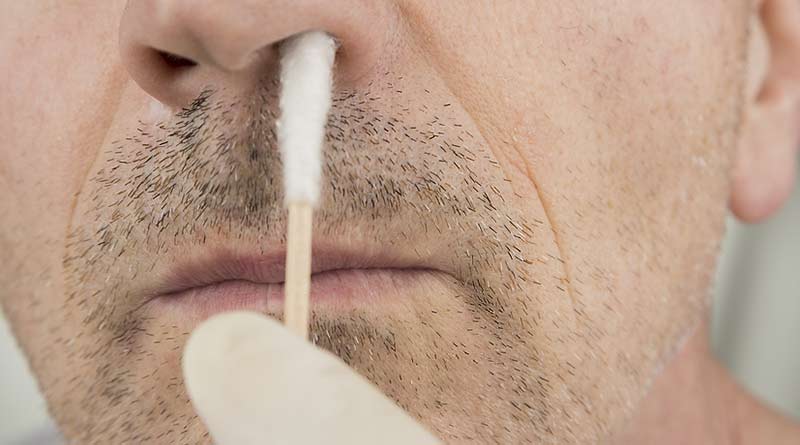
Testing for current presence of the disease requires a swab to collect a sample from inside the nose, or the back of the throat, of an individual. When we see media pictures of people attending drive through testing clinics, this is the test being done to answer the question “does this person have the virus right now?” The answer to this question can be provided within hours.
B) Antibody (serological test).
Serological tests are blood tests that look for antibodies in the blood. These tests typically involve just a finger prick of blood, which is applied to a testing strip. These tests can be done at home. This is the test being done to answer the question “has this person had the virus?” The answer to this question can be provided within 15-20 minutes.
There are many limitations of test A. The test is only as good as the sample and so the swab needs to be of high quality. There is already some evidence to show that samples from sputum (saliva and mucus coughed up) produce the most accurate result (Ref 9). The sample also needs to have been handled and stored properly. The test can only identify people with active infection; individuals tested in the incubation period, before the virus really takes hold, can test negative and individuals within the recovery period of COVID-19 will likely test negative.
There are many limitations of test B. Antibody tests generally are problematic because a number of antibodies can react to the reagent cells tested and mask the antibody of interest. Specifically, it can take approximately 14 days for antibodies to COVID-19 to appear (Ref 10). Testing someone during this window will produce a negative result.
Test accuracy
With COVID-19, for A, it is important to know who has the virus right now, so that they can be isolated/treated accordingly. It is so important not to miss any true positives, that false positives should be accepted as a necessary consequence. The sensitivity for this test needs to be high. This does mean that some people will be diagnosed with COVID-19 who don’t have it.
With COVID-19, for B, it is important to know who has not had the disease. It would be more harmful to think that someone is immune when they aren’t. For this test, therefore, it is so important not to allow false positives, that a number of false negatives need to be accepted. The specificity for this test needs to be high. This does mean that some people will be diagnosed as not having had COVID-19 when in fact they have had it.
There is limited evidence on the accuracy of either COVID-19 test at the moment, but the evidence that we do have raises concerns.
Regarding A), the tests to confirm who currently has the virus, I have come across only two academic papers about the test accuracy and neither is robust.
The first, published on March 5th, has been withdrawn already (Ref 11). No reason has been given for the withdrawal. The full paper has not been made available at any time. The abstract reported that the positive predictive value – the probability that people with a positive test actually have the virus – was only 20%. The false positives were reported as 80%. The numbers in this paper must be disregarded, as it has been withdrawn, but the paper indicates that false positives might be high.
A second paper has been made available online, while going through peer review in parallel (Ref 12). This is happening often with COVID-19 papers. Journals have taken the view that any information is better than no information, even if the paper doesn’t subsequently get through peer review. This second paper suggests that the test for the virus may give false negatives approximately 30% of the time. An article in the New York Times by Dr. Harlan Krumholz, a professor of medicine at Yale University, advises people to assume that they have the virus if they have the symptoms, even if they test negative (Ref 13). The false negative issue has been confirmed in other articles. There have been reports of some people testing negative several times even though they were infected with the virus (Ref 14).
Regarding B), this is the test that would be invaluable to undertake in large sections of the population. This, if accurate, would help governments to understand the degree of immunity that the population has developed and to be able to identify individuals who could help others more safely (as they would not be at risk of passing on the virus).
Test B is where we have the biggest test accuracy issues. The transcript of the UK government briefing on April 3rd, quoted the Health Secretary, Matt Hancock, as saying: “And, in fact, on the G7 call earlier, it’s clear that no G7 country has yet found a home antibody test, that works. But we continue to search for one” (Ref 15).
On April 3rd, the US FDA officially authorized its first serological antibody blood test for COVID-19 (Ref 16). The UK government is reported to be working with nine companies, in the hope that at least one reliable antibody test can be put into operation (Ref 17).
In conclusion
“Test, test, test” is the right strategy in principle, but, in practice, test limitations need to be accounted for. Governments and medical advisors are being attacked for not testing enough, while little is being said about the limitations of those tests.
We need to know who has the virus right now and thus we need to be prepared to diagnose some people with COVID-19 who don’t have it – to err on the side of caution. The very limited academic evidence that we have so far on this test is poor and inconsistent.
We need to know who has had the virus already and thus we need to be prepared to miss some people who have had COVID-19 – to err on the side of caution. The official UK government document on testing notes that “No government in the world has yet rolled out a full COVID-19 antibody testing programme” (Ref 18). The same document cautions that “Our experts are clear that an unreliable test is worse than no test.”
I’m not sure that I agree with the “unreliable test is worse than no test” caution. Some information must be better than no information when information is so valuable right now. Provided that we know the principles of tests – true and false positives and true and false negatives – and provided that we know the side of caution to err upon, we can make relatively informed decisions from relatively little information.
We may also need to apply some common sense in the absence of robust lab tests. A young A&E doctor in our wider family, working with patients with COVID-19, developed a persistent cough, high temperature and extraordinary fatigue. She wasn’t tested for COVID-19, but you could put big money on the fact that she had it. She’s back at work already and so we can now assume that she’s in the group of people who have had COVID-19. How can we gather all such information?
As for the numbers who have had it, I come back to that tweet on March 13th: “Can anyone explain how a virus (identified in Wuhan in Dec 2019) spread to the Canadian prime minister’s wife, one of Hollywood’s top actors & his wife, a Premier League football manager, and a British member of parliament – within 16 weeks – while bypassing the majority of us?” (Ref 19). The answer is, of course, it didn’t. Many of us have had the virus already.
The UK has just issued a call to arms for people with modelling skills (Ref 20). Maybe artificial intelligence models can work out how many people have had the virus already such that Prince Charles, Idris Elba and Pink have all had it. What can the concept of “six degrees of separation” tell us right now?
References
Ref 1: https://edition.cnn.com/2020/03/30/world/coronavirus-who-masks-recommendation-trnd/index.html
Ref 2: https://www.smh.com.au/national/world-health-organisation-reviews-face-mask-evidence-20200402-p54gjz.html
Ref 3: https://www.scmp.com/news/china/article/3078407/coronavirus-world-health-organisation-reverses-course-now-supports
Ref 4: https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/cloth-face-cover.html
Ref 5: https://metro.co.uk/2020/04/03/government-still-wont-recommend-wearing-face-masks-public-12506422/
Ref 6: https://www.who.int/dg/speeches/detail/who-director-general-s-opening-remarks-at-the-media-briefing-on-covid-19—16-march-2020
Ref 7: Parikh et al. Understanding and using sensitivity, specificity and predictive values. Indian J Ophthalmol. 2008. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2636062/
Ref 8: https://www.abpi.org.uk/medicine-discovery/covid-19/briefing-coronavirus-covid-19-testing/
Ref 9: Yang et al. Evaluating the accuracy of different respiratory specimens in the laboratory diagnosis and monitoring the viral shedding of 2019-nCoV infections. Currently in peer review. April 2020. https://www.medrxiv.org/content/10.1101/2020.02.11.20021493v2.full.pdf
Ref 10: Okba et al. SARS-CoV-2 specific antibody responses in COVID-19 patients. March 2020. https://www.medrxiv.org/content/10.1101/2020.03.18.20038059v1.full.pdf
Ref 11: Zhuang et al. [WITHDRAWN: Potential False-Positive Rate Among the ‘Asymptomatic Infected Individuals’ in Close Contacts of COVID-19 Patients] March 2020. https://pubmed.ncbi.nlm.nih.gov/32133832/
Ref 12: Yang et al. Evaluating the accuracy of different respiratory specimens in the laboratory diagnosis and monitoring the viral shedding of 2019-nCoV infections. Currently in peer review. April 2020. https://www.medrxiv.org/content/10.1101/2020.02.11.20021493v2.full.pdf
Ref 13: https://www.nytimes.com/2020/04/01/well/live/coronavirus-symptoms-tests-false-negative.html
Ref 14: https://www.medicinenet.com/script/main/art.asp?articlekey=228250
Ref 15: (At 31.52) https://www.rev.com/blog/transcripts/united-kingdom-covid-19-briefing-transcript-april-3 (The G7 countries are Canada, France, Germany, Italy, Japan, UK and US).
Ref 16: https://www.fiercebiotech.com/medtech/fda-officially-authorizes-its-first-serological-antibody-blood-test-for-covid-19
Ref 17: https://www.bbc.co.uk/news/uk-52140376
Ref 18: https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/878121/coronavirus-covid-19-testing-strategy.pdf
Ref 19: https://twitter.com/DavidVidecette/status/1238487118030258180
Ref 20: https://royalsociety.org/news/2020/03/Urgent-call-epidemic-modelling/




I’m with mjwillyone here. It is all a much ado about nothing. I can see no evidence that this virus is any worse than seasonal flu but I’m sure that time will tell. What is coming to light is the way that hospitals in different countries treat COVID-19. We have always maintained that taking vitamin C, D3 and quercetin is a good way to protect yourself from seasonal colds and flu and COVID-19 seems to be no different. We need to stop listening to the hype and start looking at the figures. Give me input Stephanie.
I have never seen a panic amid such lack of medical research before in my lifetime. Wouldn’t it have been better to quarantine the elderly and others most susceptible to harm than so much of the healthy US working population? I hear I am to receive money from the government when my job is not at risk at all? Here we are spending in one stroke of a pen the equivalent of about 1/10 the debt of US government to help the US economy. I blame the government for not finding accurate information and thinking sensibly so as to protect the most likely to be harmed by giving a pass to others.
Now I watch as those who go shopping with 2-3 family members vilified for not reducing their numbers… after all this is 2/3 more people than need to be out infecting others! Why haven’t we responded this way with the flu, with SARS, with Ebola??
Give us the science that was used to support this ridiculous response to this infection! I have seen that those most likely to over respond are those that rely on the news media for their spoonful of “truth.”
I do feel for those physically effected. But I also feel for those who are forced to stop working, though healthy, because of the action of governments making rulings real research support.
Dear Zoe,
Great article again, but I think we need to swap around the sensitivities and specificities
For Test A, we need to be certain not to miss a single COVID positive individual .
We must therefore ensure we have no false negatives and so a high specificity is required to rule the disease in -SpPIn.
For Test B, we need to rule the diagnosis out and we therefore need a high sensitivity – SnNout.
Its terribly counter intuitive, but I think SpPin and SnNOut are what’s required !
https://www.cebm.net/2014/03/sppin-and-snnout/
BW
John
Hi John
Many thanks for this. So sorry I missed replying to it sooner!
I’m familiar with SpPIN and SnNOUT (or twist and shout as I remember them!) They were in that fab paper ref 7 (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2636062/)
I think I’ve got it the right way round, but it may help to remove the two sentences “The sensitivity for this test needs to be high” (A) and “The specificity for this test needs to be high” (B) if they might confuse…
SpPIN: a highly Specific test if Positive, rules IN disease. Specificity is d/(b+d) i.e. if b is zero, then d is 100%. B is false positives.
SnNOUT: a highly Sensitive test if Negative, rules OUT disease. Sensitivity is a/(a+c) i.e. if c is zero, then a is 100%. C is false negatives.
I think of SpPIN and SnNOUT as working horizontally in the 2×2 table. If a SpPIN test is positive, false positives (b) are low and so someone testing positive is likely to have the disease (box a). If a SnNOUT test is negative, false negatives are low (c) and so someone testing negative is likely to not have the disease (box d).
For A, virus now, we don’t want false negatives (c) and we’ll accept false positives (b) to achieve this. Hence c should be as low as possible -> highly sensitive test.
For B, virus in the past, we don’t want false positives (b) and we’ll accept false negatives (c) to achieve this. Hence b should be as low as possible -> highly specific test.
I think that’s right, but happy to amend if not or just delete those two sentences if they confuse.
Thanks again
Best wishes – Zoe
Note:- Not my research but thought people might find it interesting and VERY enlightening.
________________________________________________________________________________________________-
Chicago Tribune, April 3: “A new, different type of coronavirus test is coming that will help significantly in the fight to quell the COVID-19 pandemic, doctors and scientists say.”
“The first so-called serology test, which detects antibodies to the virus rather than the virus itself, was given emergency approval Thursday by the U.S. Food and Drug Administration.”
“The serology test involves taking a blood sample and determining if it contains the antibodies that fight the virus. A positive result indicates the person had the virus in the past and is currently immune.”
“Dr. Elizabeth McNally, director of the Northwestern University Feinberg School of Medicine Center for Genetic Medicine…’You’ll see many of these roll out in the next couple of weeks, and it’s great, and it will really help a lot,’ said McNally, noting doctors and scientists will be able to use it to determine just how widespread the disease is, who can safely return to work and possibly how to develop new treatments for those who are ill.”
Got that? A positive test means the patient is now immune to the virus and can walk outside and go back to work.
NBC News, April 4, has a somewhat different take: “David Kroll, a professor of pharmacology at the University of Colorado who has worked on antibody testing, explained that the antibodies [a positive test] mean ‘your immune system [has] remembered the virus to the point that it makes these antibodies that could inactivate any future viral infections’.”
“What the test can’t do is tell you whether you’re currently sick with coronavirus, whether you’re contagious, whether you’re fully immune – and whether you’re safe to go back out in public.”
“Because the test can’t be used as a diagnostic test, it would need to be combined with other information to determine if a person is sick with COVID-19.”
Oops. No, this really isn’t a diagnostic test, it doesn’t tell whether the patient is immune and can go back to work. Excuse me, what??
Business Insider, April 3: “The world’s leading industrial nations have so far failed to identify any coronavirus antibody tests that will be accurate enough for home use, according to the UK’s Health Secretary Matt Hancock.”
“The UK and other nations are currently examining plans to use antibody tests to allow individuals with immunity to COVID-19 to exit their national lockdowns early through the use of a so-called ‘immunity passport’.”
“Spain was recently forced to return tens of thousands of rapid coronavirus tests from a Chinese company after they were found to be accurate just 30% of the time.”
“Some tests have demonstrated false positives, detecting antibodies to much more common coronaviruses.”
“Scientists also remain unsure about the extent to which a past infection could prevent reinfection and how long an immunity would remain.”
Hmm. So the new antibody test has very serious problems, and it hasn’t been cleared for public use.
Medicine Net (undated): “Researchers at the Mount Sinai Health System say they’ve developed a test that can find out if you already have had or were infected with the new coronavirus.”
“The test is called “serological enzyme-linked immunosorbent assay,” or ELISA for short. It checks whether or not you have antibodies in your blood to SARS-CoV-2, the scientific name of the new coronavirus that causes COVID-19.”
“Researchers say ELISA works like antibody tests for other viruses, such as hepatitis B. It will show whether your immune system — the body’s defense against germs — made contact with SARS-CoV-2, even months before.”
“The test could help scientists fight the pandemic in several ways. It can give researchers a more accurate measure of how many people had the new coronavirus. It would also let health care workers who were ill with COVID-19 symptoms, but were never tested for the disease, return to work — confident that they are now immune.”
So wait, it’s a great test. Right? A positive test result indicates immunity, and people can return to work. What??
Science News, March 27: “The United Kingdom has ordered 3.5 million antibody tests, which would show whether someone has been exposed to COVID-19. Such tests, which just take a drop of blood, could help reveal people who have been exposed to the virus and are now likely immune, meaning they could go back to work and resume their normal lives.”
“Science News spoke with David Weiner, director of the Vaccine and Immunotherapy Center at the Wistar Institute in Philadelphia, and Charles Cairns, dean of the Drexel University College of Medicine, about how antibody tests work and what are some of the challenges of developing the tests.”
“Cairns: ‘The big question is: Does a positive response for the antibodies mean that person is actively infected, or that they have been infected in the past? The tests need to be accurate, and avoid both false positives and false negatives. That’s the challenge’.”
Oops again. Cairns is saying the new test, if it reads positive, might mean the person is infected now. Or it might mean they were infected—and are now presumably immune. Figuring out which is the challenge. No kidding. It’s the difference between sick and healthy. So a positive test result means the patient is sick OR healthy.
As a reference, let’s look at how this same antibody test has been used in the past. For example, in the case of hepatitis A:
URMC Rochester (undated): This test looks for antibodies in your blood called IgM. The test can find out whether you are infected with the hepatitis A virus (HAV)…If your test is positive or reactive, it may mean: You have an active HAV infection…You have had an HAV infection within the last 6 months.”
In other words, a positive antibody test could mean you’re sick now, or were once sick but are presumably immune now. Wonderful.
Medscape comments on the meaning of a positive antibody test for the Zika virus: “…immunoglobulin (Ig) M and neutralizing antibody testing can identify additional recent Zika virus infections…However, Zika virus antibody test results can be difficult to interpret because of cross-reactivity with other flaviviruses…”
Two things here: no word about a positive test result revealing IMMUNITY from Zika; and a warning that a positive test might not have anything to do with Zika at all—that’s what “cross-reactivity” means.
Medlineplus, referring to a Zika “blood test,” which would include antibody testing, states, “A positive Zika test result probably means you have a Zika infection.” Not immunity.
And there you have it. The official word on the COVID antibody test from official sources. It’s yes, no, and maybe. Public health officials can SAY whatever they want to about antibody tests: a positive result means you’re immune, it means you have an infection, it means you’re walking on the moon eating a hot dog.
Generally speaking, before 1984 a positive antibody test was taken to mean the patient had achieved immunity from a germ. After 1984, the science was turned upside down; a positive result meant the patient “had the germ” and was not immune. Now, with COVID-19, if you just read news headlines, a positive test means the patient is immune; but if you read down a few paragraphs, a positive test means the patient is maybe…maybe not…immune. Maybe infected, maybe not infected. Maybe sick, maybe not sick. And, on top of all that, antibody tests are known to read falsely positive, owing to factors that have nothing to do with the virus being tested for.
Nailed them, with their own words from official sources about their own diagnostic test for the coronavirus with fatal flaws in the test.
Because case numbers are based on those tests (or no tests at all), the whole “pandemic effect” has been created out of thin air.
The widespread test for the COVID-19 virus is called the PCR, let’s go to published official literature, and see what it reveals. Spoiler alert: the admitted holes and shortcomings of the test are devastating.
From “CDC 2019-Novel Coronavirus (2019-nCoV) Real-Time RT-PCR Diagnostic Panel”:
“Detection of viral RNA may not indicate the presence of infectious virus or that 2019-nCoV is the causative agent for clinical symptoms.”
Translation: A positive test doesn’t guarantee that the COVID virus is causing infection at all. And, ahem, reading between the lines, maybe the COVID virus might not be in the patient’s body at all, either.
From the World Health Organization (WHO): “Coronavirus disease (COVID-19) technical guidance: Laboratory testing for 2019-nCoV in humans”:
“Several assays that detect the 2019-nCoV have been and are currently under development, both in-house and commercially. Some assays may detect only the novel virus [COVID] and some may also detect other strains (e.g. SARS-CoV) that are genetically similar.”
Translation: Some PCR tests register positive for types of coronavirus that have nothing to do with COVID—including plain old coronas that cause nothing more than a cold.
The WHO document adds this little piece: “Protocol use limitations: Optional clinical specimens for testing has [have] not yet been validated.”
Translation: We’re not sure which tissue samples to take from the patient, in order for the test to have any validity.
From the FDA: “LabCorp COVID-19RT-PCR test EUA Summary: ACCELERATED EMERGENCY USE AUTHORIZATION (EUA) SUMMARYCOVID-19 RT-PCR TEST (LABORATORY CORPORATION OF AMERICA)” [3]:
“…The SARS-CoV-2RNA [COVID virus] is generally detectable in respiratory specimens during the acute phase of infection. Positive results are indicative of the presence of SARS-CoV-2 RNA; clinical correlation with patient history and other diagnostic information is necessary to determine patient infection status…THE AGENT DETECTED MAY NOT BE THE DEFINITE CAUSE OF DISEASE (CAPS are mine). Laboratories within the United States and its territories are required to report all positive results to the appropriate public health authorities.”
Translation: On the one hand, we claim the test can “generally” detect the presence of the COVID virus in a patient. But we admit that “the agent detected” on the test, by which we mean COVID, “may not be the definite cause of disease.” We also admit that, unless the patient has an acute infection, we can’t find COVID. Therefore, the idea of “asymptomatic patients” confirmed by the test is nonsense. And even though a positive test for COVID may not indicate the actual cause of disease, all positive tests must be reported—and they will be counted as “COVID cases.” Regardless.
From a manufacturer of PCR test kit elements, Creative Diagnostics, “SARS-CoV-2 Coronavirus Multiplex RT-qPCR Kit”:
“Regulatory status: For research use only, not for use in diagnostic procedures.”
Translation: Don’t use the test result alone to diagnose infection or disease. Oops.
“non-specific interference of Influenza A Virus (H1N1), Influenza B Virus (Yamagata), Respiratory Syncytial Virus (type B), Respiratory Adenovirus (type 3, type 7), Parainfluenza Virus (type 2), Mycoplasma Pneumoniae, Chlamydia Pneumoniae, etc.”
Translation: Although this company states the test can detect COVID, it also states the test can read FALSELY positive if the patient has one of a number of other irrelevant viruses in his body. What is the test proving, then? Who knows? Flip a coin.
“Application Qualitative”
Translation: This clearly means the test is not suited to detect how much virus is in the patient’s body. I’ll cover how important this admission is in a minute.
“The detection result of this product is only for clinical reference, and it should not be used as the only evidence for clinical diagnosis and treatment. The clinical management of patients should be considered in combination with their symptoms/signs, history, other laboratory tests and treatment responses. The detection results should not be directly used as the evidence for clinical diagnosis, and are only for the reference of clinicians.”
Translation: Don’t use the test as the exclusive basis for diagnosing a person with COVID. And yet, this is exactly what health authorities are doing all over the world. All positive tests must be reported to government agencies, and they are counted as COVID cases.”
Those quotes, from official government and testing sources, torpedo the whole “scientific” basis of the test.
And now, I’ll add another, lethal blow: the test has never been validated properly as an instrument to detect disease. Even assuming it can detect the presence of the COVID virus in a patient, it doesn’t show HOW MUCH virus is in the body. And that is key, because in order to even begin talking about actual illness in the real world, not in a lab, the patient would need to have millions and millions of the virus actively replicating in his body.
Proponents of the test assert that it CAN measure how much virus is in the body. To which I reply: prove it.
Prove it in a way it should have been proven decades ago—but never was.
Take five hundred people and remove tissue samples from them. The people who take the samples do NOT do the test. The testers will never know who the patients are and what condition they’re in.
The testers run their PCR on the tissue samples. In each case, they say which virus they found and HOW MUCH of it they found.
“All right, in patients 24, 46, 65, 76, 87, and 93 we found a great deal of virus.”
Now we un-blind those patients. They should all be sick, because they have so much virus replicating in their bodies. Are they sick? Are they running marathons? Let’s find out.
This OBVIOUS vetting of the test has never been done. That is an enormous scandal. Where are the controlled test results in 500 patients, a thousand patients? Nowhere.
The test is an unproven fraud.
And, therefore, the COVID pandemic, which is supposed to be based on that test, is also a fraud.
“But…but…what about all the sick and dying people…why are they sick?” A NUMBER of conditions—none involving COVID, and most involving old traditional diseases—are making people sick.